What is ferritin and how does it affect health?
Okay, I can’t lie TikTok inspired me to write this post. I keep seeing videos of women experiencing fatigue, irritabilty or hair loss and being told by their doctor that there is no reason for their symptoms. Yet their ferritin level is very low.
This happen to me. I was struggling to concentrate and was loosing a lot of hair. My doctor ran some blood tests and told me everything was “normal”, despite my ferritin being 16 ug/L.
I hope this post sheds some light on what ferritin is, how both low and high ferritin levels may your impact health and what you can do about it. As always, I have packed this post with information so feel free to skim read and skip to the subheadings that are most relevant to you.
What is ferritin?
Ferritin is a protein that takes in excess iron from cells and stores it for future use, releasing the iron when the body needs it.
Ferritin levels can indicate iron status, inflammation levels, infection and certain cancers.
Interpreting ferritin levels on a blood test
Conventional reference ranges for ferritin:
• For females 15 – 200 ug/L
• For males 15 – 300 ug/L
Reference ranges can vary slightly from lab to lab. For example, NHS North Bristol state the adult referrence range for ferritin as 11 – 310 ug/L and 24 – 340 ug/L for females and males, respectively.
These are large reference ranges based on values observed in 95% of a population sample. These range of values represent what is common, not what is healthy.
You may wonder why reference ranges don’t reflect optimal health. This is because they are designed to detect clear disease states, such as iron deficiency anaemia, rather than earlier or subclinical deficiencies such as iron deficiency without anaemia. Conventional medicine tends to focus on diagnosing and treating disease, rather than on health optimisation or disease prevention.
As a nutritional therapist I use functional medicine reference ranges, which research shows is what the body needs for optimal health. Therefore, these reference ranges are narrower.
Functional medicine reference ranges for ferritin:
• For females and males 70 – 100 ug/L
Low ferritin levels
From a functional persceptive when ferritin drops below 50 ug/L symptoms may start to appear. For example you may feel persistent fatigue despite rest. Many researchers have argued that the cut off defining iron deficiency without anaemia should be raised from 15 ug/L to 50 ug/L.
When your ferritin is ≤30 ug/L this is considered iron deficiency without anaemia.
The UK’s NICE guidelines state:
“In all people, a serum ferritin level of less than 30 micrograms/L confirms a diagnosis of iron deficiency. Low levels of ferritin can result in symptomatic and functional impairment even in those individuals with a normal haemoglobin, especially in women who are menstruating.”
However, low ferritin alone does not necessarily mean you need to supplement. Ferritin should always be interepreted as part of a full iron panel, as well as considering symptoms.
Full iron panel:
- Serum iron – the amount of iron in your blood
- Serum ferritin – the amount of iron stored in your body
- TIBC (Total iron binding capacity) – the blood’s capacity to bind iron with transferrin, a protein that transports iron
- Transferrin saturation – how much iron is currently bound to transferrin
Symptoms of low ferritin include:
- Pale skin/ lips/ gums
- Fatigue and weakness
- Decreased athletic performance
- Dizziness
- Poor nail quality
- Hair shredding and hair loss
- Shortness of breath
- Rapid heart rate
- Headache
- Irritability
- Cold hands and feet
- Increased bruising
Causes of low ferritin include:
- Blood loss – heavy periods, shorter menstraul cycles under 21 days, surgery, trauma
- Insufficent iron in your diet – more common in vegans and vegetarians
- Poor gastrointestinal absorption – dysbiosis, small intestinal bacterial or fungal overgrowth (SIBO/ SIFO), Helicobacter Pylori, IBD, Coeliac disease
- Insufficient stomach acid (hypochlorhydria)
- Parasitic infection – some paraistes such as Hookworm feed on blood as they need iron for survival
- Endurance sports – iron can be lost in sweat
- Pregancy and lactation – demand for iron greatly increases
- Internal bleeding
How to increase ferritin and iron levels
Increase your intake of iron rich foods. Dietary iron comes in two forms: heme iron, found in meat, poultry, and fish, which is more easily absorbed; and non-heme iron, found in plant foods.
Sources of dietary iron:
- Beef
- Liver (avoid during pregnancy)
- Shellfish
- Beans and legumes – lentils, kidney beans, chickpeas
- Tofu
- Dried apricots
- Broccoli
- Leafy green vegetables
- Blackstrap molasses
The recommend daily intake of iron is:
• Menstrauting females: 14.8 mg
• Pregnancy: 27 mg
• Males and non-menstruating females: 8.7 mg
Tips to help maximise iron absorption from food:
- Enjoy coffee, tea, or green tea away from iron-rich meals, as these can reduce iron absorption.
- Add a source of vitamin C to your meal to enhance absorption, such as kiwi, strawberries, bell peppers, or a squeeze of lemon or lime juice.
Iron supplementation. Only supplement with iron if your iron levels have been tested and you’ve been advised that you are iron deficient.
If supplementation is needed, look for iron bisglycinate (ferrous bisglycinate). This form is generally better absorbed and less likely to cause constipation compared with ferrous fumarate or ferrous sulfate. Choosing a supplement that also contains vitamin C can further enhance iron absorption. For example, ‘Easy iron by Terranova‘ or ‘Gentle iron and vitamin C by Dr.Vegan‘.
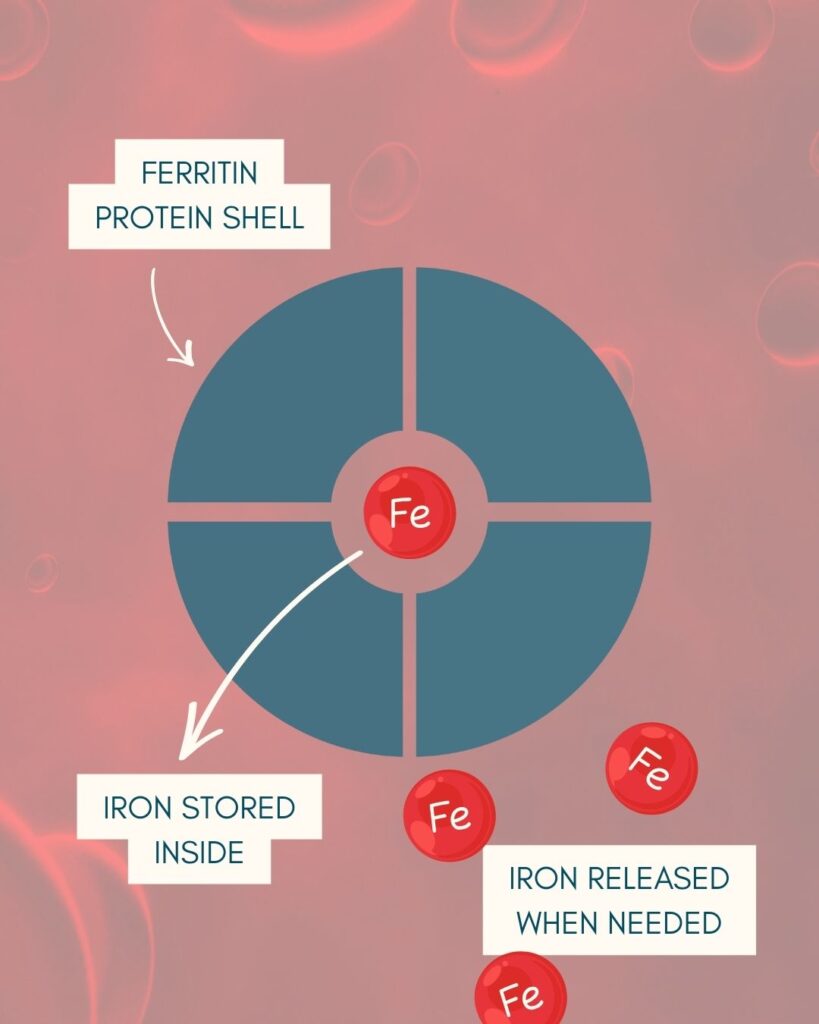
Simple depiction of ferritin
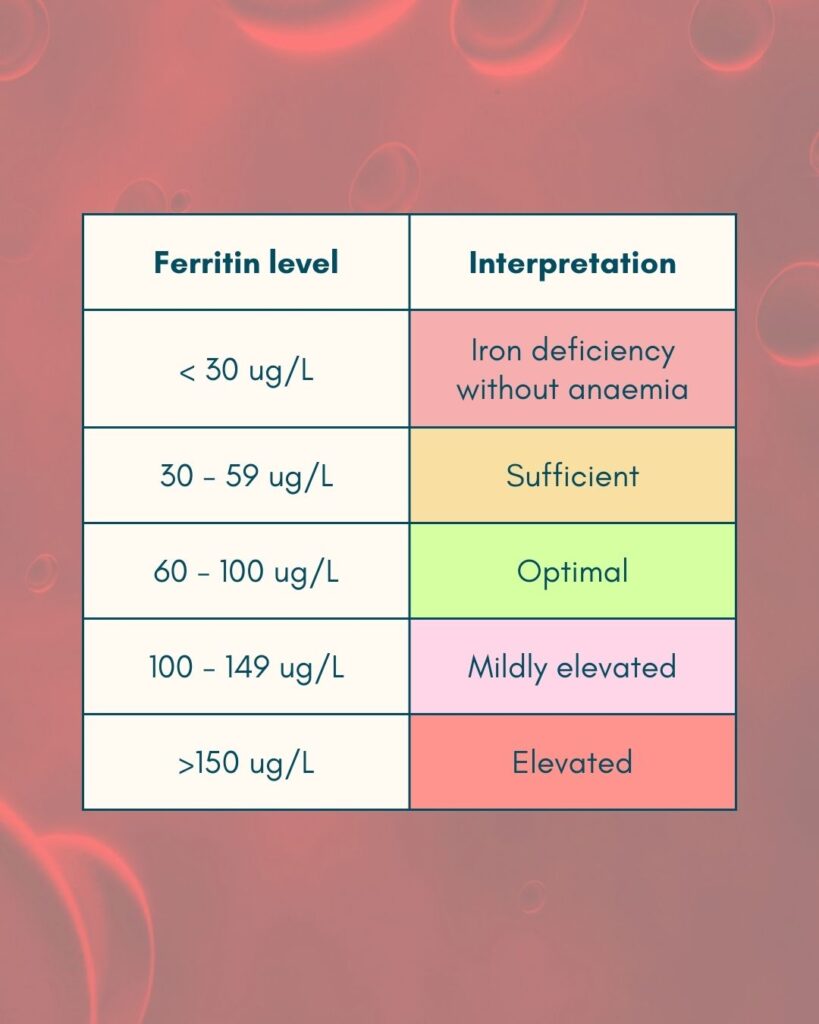
Reference ranges from a functional medicine perspective
High ferritin levels
Too much iron can be just as problematic as too little. Excess iron is toxic and can damage cells.
The World Health Organization states:
“A ferritin concentration exceeding 150 µg/L in menstruating women and 200 µg/L in men and non-menstruating women who are otherwise healthy may indicate a risk of iron overload .”
Symptoms of high ferritin include:
- Fatigue and weakness
- Joint pain
- Abdominal pain
- Heart palpitations
Causes of high ferritin may include:
- Inflammation – e.g. from metabolic disorders like type 2 diabetes, autoimmune conditions or infection
- Hyperthyroidism
- Liver damage
- Alcohol misuse
- Repeated blood transfusions
- Excess dietary iron or supplementation
- Haemochromatosis – a genetic condition where the body absorbs excess iron
- Cancer
How to lower ferritin and iron levels
Firstly, the cause of high ferritin and/or iron needs to be established. Your doctor may conduct the following investigations to establish the cause:
- Full blood count
- Liver function test
- Full iron panel
- CRP (C-reactive protein) – a marker of inflammation
If iron overload is a concern, strategies to help lower iron levels include:
- Reducing intake of iron rich foods (see above for examples)
- Increasing intake of foods that inhibit iron absorption, such as dairy products, coffee, tea, cocoa, wholegrains, beans, and legumes
- Donating blood, where appropriate and medically approved
Home testing options for ferritin
If for whatever reason your are unable to obtain your iron levels from your doctor there are home tesing options.
I would recommend a venous blood draw rather than a finger-prick test. Finger-prick tests collect a very small capillary blood sample and can be less reliable when assessing iron status. A venous blood draw provides a larger sample from a vein, which generally allows for greater accuracy and more reliable results.
Home testing options for ferritin and iron include:
References
Cancado, R. D., Leite, L. A. C., & Muñoz, M. (2025). Defining Global Thresholds for Serum Ferritin: A Challenging Mission in Establishing the Iron Deficiency Diagnosis in This Era of Striving for Health Equity. Diagnostics (Basel, Switzerland), 15(3), 289. https://doi.org/10.3390/diagnostics15030289
Kotla, N. K., Dutta, P., Parimi, S., & Das, N. K. (2022). The Role of Ferritin in Health and Disease: Recent Advances and Understandings. Metabolites, 12(7), 609. https://doi.org/10.3390/metabo12070609
Knowler, K. (2020). Blood labs: a guide to interpreting blood test results for fatigue.
Lambert Sports Clinic. (2025, Jan). Finger-Prick vs Venous Blood Tests: Why Accuracy Matters for Your Health Decisions. https://lambertsportsclinic.co.uk/blog/finger-prick-vs-venous-blood-tests.html
Martens, K., & DeLoughery, T. G. (2023). Sex, lies, and iron deficiency: a call to change ferritin reference ranges. Hematology. American Society of Hematology. Education Program, 2023(1), 617–621. https://doi.org/10.1182/hematology.2023000494
National Heart, Lung, and blood Institiute. (2022, Mar 24). Iron-Deficiency Anemia. https://www.nhlbi.nih.gov/health/anemia/iron-deficiency-anemia
NICE. (2025, Oct). Anaemia – iron deficiency: What investigations should I arrange to confirm iron deficiency anaemia? https://cks.nice.org.uk/topics/anaemia-iron-deficiency/diagnosis/investigations/
NHS. (2020, Aug 3). Iron: vitamins and minerals. https://www.nhs.uk/conditions/vitamins-and-minerals/iron/
NHS, North Bristol. (2025, Feb). Ferritin. https://www.nbt.nhs.uk/severn-pathology/requesting/test-information/ferritin
World health organization (WHO). (2023, Aug 9). Use of ferritin concentrations to assess iron status in individuals and populations. https://www.who.int/tools/elena/interventions/ferritin-concentrations